Overview of the Global Anemia Problem, Including Iron Deficiency Anemia
The World Health Organization (WHO) defines anemia among women of childbearing age as the condition of having a hemoglobin concentration of < 12.0 g/dL at sea level; among pregnant women it is defined as < 11.0 g/dL. The hemoglobin concentration cutoff level that defines anemia varies by age, gender, physiological status, smoking status, and the altitude at which the assessed population lives.
The primary cause of anemia is iron deficiency, a condition caused by inadequate intake or low absorption of iron, the increased demands of repeated pregnancies—particularly if not well spaced (e.g., fewer than 36 months between pregnancies)—and loss of iron through menstruation. Other causes of anemia include vitamin deficiencies (such as a deficiency of folic acid or vitamin A), genetic disorders, malaria, parasitic infections, HIV, tuberculosis, common infections, and other inflammatory conditions. While iron deficiency anemia (IDA) accounts for about onehalf of all anemia cases, it often coexists with these other causes.
Iron deficiency anemia is most common during pregnancy and in infancy, when physiological iron requirements are the highest and the amount of iron absorbed from the diet is not sufficient to meet many individuals’ requirements (Stoltzfus and Dreyfuss 1998). Anemia’s effects include increased risk of premature delivery, increased risk of maternal and child mortality, negative impacts on the cognitive and physical development of children, and reduced physical stamina and productivity of people of all ages (Horton and Ross 2003). Globally, IDA annually contributes to over 100,000 maternal deaths (22 percent of all maternal deaths) and over 600,000 perinatal deaths (Stoltzfus, Mullany, and Black 2004). Key anemia control interventions include promoting a diversified diet, iron-folic acid (IFA) supplementation during pregnancy, iron fortification of staple foods, prevention and treatment of malaria, use of insecticide-treated bed nets, helminth prevention and control, delayed cord clamping, and increased birth spacing.
Maternal Anemia in Rwanda
The prevalence rate of anemia among pregnant women and women of child-bearing age in Rwanda is 19.5 and 17 percent, respectively, making anemia a mild public health problem among these groups of women as defined by WHO standards1 (NISR, MOH, and ICF International 2012) The highest prevalence of anemia (22.8 percent) is in East Province, where it is classified as a moderate public health concern. Regarding anemia severity, the majority of cases among pregnant women in country are classified as mild or moderate, while less than one percent of this population is diagnosed as severe.2
Falter Points in Women's Consumption of Iron-Folic Acid During Pregnancy
WHO recommends that all pregnant women receive a standard dose of 30–60 mg iron and 400 μg folic acid beginning as soon as possible during gestation (WHO 2012). Ideally, women should receive iron-containing supplements no later than the first trimester of pregnancy, which means ideally taking 180 tablets before delivery. It is important to note, that many countries aim for women to receive 90 or more tablets during pregnancy.
Figure 1 on the following page shows a decision-tree analysis of how well the Rwandan antenatal care (ANC) system distributes IFA, and identifies four potential points at which the system might falter (highlighted in orange). The figure tracks the number and percentage of women who obtained ANC, those who subsequently received and consumed at least one IFA tablet, and those who consumed the ideal minimum number of tablets.3 All data are based on Rwanda Demographic and Health Survey (RDHS) questions that were asked of women who were in a permanent union and had been pregnant in the five years prior to being interviewed4 (NISR, MOH, and ICF International 2012).
Figure 1. Analysis of Falter Points Related to Distribution and Consumption of IFA through Rwanda’s ANC Program in 2011, Women of Reproductive Age (15–49 Years) n = 13,671
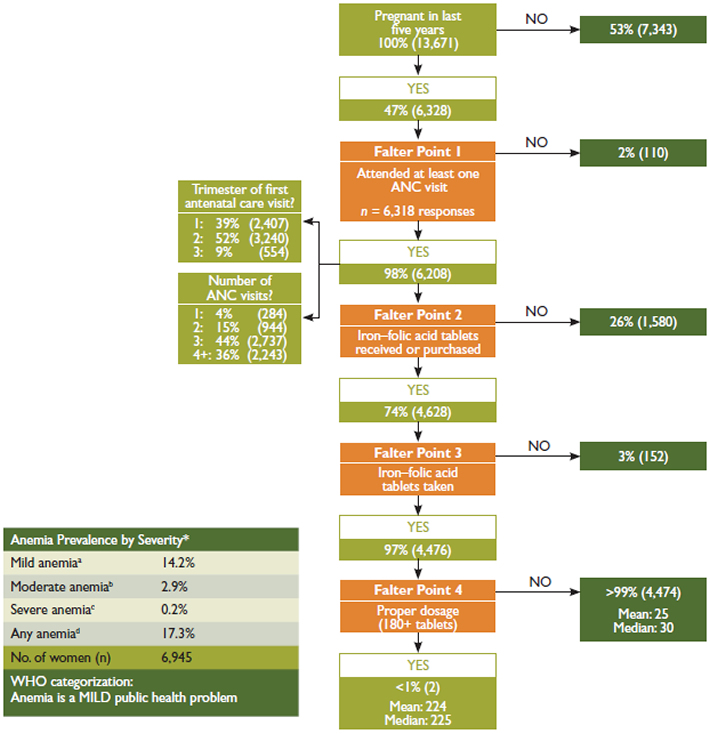
Main Conclusions: Rwanda’s high ANC coverage makes it a strong vehicle for IFA distribution. Still, among women who were pregnant in the last five years, had at least one ANC visit, and took at least one IFA tablet, less than one percent received and took the ideal minimum number of tablets. Both supply and demand need to be investigated.
Anemia levels are current at the time of the DHS. All other data in the schematic covers the last pregnancy in the five years prior to the DHS.
*Percent of women 15–49 based on Hemoglobin levels Hb (g/dL)
aNPW 11.0≤Hb≤11.9, PW 10≤Hb≤10.9 bNPW 8.0≤Hb≤10.9, PW 7.0≤Hb≤9.9 cNPW Hb<8.0, PW Hb<7.0 dNPW Hb<12, PW Hb<11
Non-responses, no data were recorded to “No” for “IFA tablets received?” and “IFA tablets taken?”; recoded to zero for “Number of tablets taken?”
Source: Calculations and anemia levels are from the Rwanda Demographic and Health Survey (2010).
Many supply-side aspects—including both adequacy of IFA tablet supplies and technical knowledge and practices of ANC providers—need to be considered when assessing how well an ANC program delivers IFA. In addition, Falter Point 4 in Figure 1 clearly shows that the provision of IFA tablets to a pregnant woman is a necessary but not sufficient condition for the woman to consume the tablets, particularly at the ideal minimum. Thus, demand-side factors also play a critical role in determining the coverage and effectiveness of this program. These include whether or not women seek antenatal care and the timing and number of visits, as well as the extent to which women are aware of the significance of anemia and IFA, ask for IFA tablets, and comply with the IFA regimen.
Understanding the relative significance of each falter point enables them to be prioritized for more in-depth analysis, providing a first step in an evidence-based approach to systematically improving the program. The DHS does not collect information on the number of IFA tablets received by women. In the case of Falter Point 4, this lack of data creates ambiguities that make it impossible to fully understand whether shortcomings of the system relate primarily to supply- or to demandside factors. Despite this limitation, the decisiontree analysis presented in Figure 1 still enables prioritizing the falter points for more in-depth analysis and action at the national, district, and health center levels.
Analysis of Falter Points
Falter Point 1:
Did not attend at least on ANC visit
Only two percent of women did not obtain at least one ANC visit.
ANC’s high coverage makes it a strong vehicle for providing IFA.
Falter Point 2:
Did not receive or purchase at least one IFA tablet
Of the women with at least one ANC visit, 26 percent did not receive or purchase any IFA.
There are several system/supply-side performance shortcomings that need additional analysis, including: (1) inadequate supply (e.g., stock outs); (2) provider knowledge; and (3) provider practices. These three factors are directly implicated in Falter Point 2, and represent the second most important falter point among all pregnant women in Rwanda.
Unfortunately, the RDHS does not report the source(s) of the IFA tablets women received or purchased. It is likely that women who attend ANC may be more likely to be aware of, to value, and also to take IFA tablets, regardless of where they obtain them. Thus, we would expect there to be a high correlation between the number of women who had at least one ANC visit and those who received or purchased IFA, which is consistent with the data. While less than one percent of Rwandan women who received or purchased IFA did not have any ANC visits (not shown), it is difficult to ascertain whether or not those who received ANC care obtained their IFA tablets from their ANC provider. What is known, however, is that women who have had one or more ANC visits and who did not receive any IFA, constitute a missed opportunity to reduce the risk of IDA among a high-risk population.
Falter Point 3:
Did not take at least one IFA tablet
Of the women who received IFA, three percent did not consume any tablets.
This demand-side constraint is relatively small and may be due to women not understanding the significance of anemia and/or the significance of IFA. This misunderstanding may reflect: (1) inadequate provider counseling and follow-up; (2) women’s beliefs about actual or possible sideeffects; or (3) sociocultural factors.
Falter Point 4:
Did not consume 180 or more IFA tablets
Of the women who received and took IFA, more than 99 percent did not consume the ideal minimum of 180 IFA tablets.
Figure 1 sheds some light on two possible causes of Falter Point 4, although further research is needed to establish their relative importance. First, 61 percent of women who received ANC began their care after the first trimester, and were therefore unlikely to receive the recommended minimum IFA regimen due to a late contact. Second, the 63 percent of women who had less than WHO’s recommended four ANC visits during their last pregnancy may have likewise started their ANC too late, or may not have had enough visits to receive and consume the 180 tablets. Both of these are likely contributing factors, and may be tied to both demand- and/or supply-side constraints.
Globally, research has found that other common causes of Falter Point 4 include: (1) providers do not have access to adequate supply; (2) women do not receive adequate tablets because they have little access to care, start ANC late, or do not have enough ANC visits making it difficult to obtain 180 tablets (given IFA distribution protocols); (3) providers do not provide adequate counseling or follow-up; and (4) women do not adhere to the regimen, which may be due to difficulty in remembering to take the tablets daily, not knowing all the tablets are necessary, fear of having a big baby, side effects, or tablet-related issues (taste, size, color, coating, packaging/storage problem). Further research is needed to determine the specific reasons for this falter point in Rwanda.
Analysis by Sociodemographic Variables and Trends Over Time
Table 1 shows variations in the coverage of the Rwandan ANC program and consumption of IFA tablets across regions, urban/rural residence, and wealth. The degree of equity across all three of the characteristics analyzed in the table is remarkable for both ANC coverage rates and the percentage of women who took at least one IFA.
The marked increases between 2005 and 2010 in the percentage of women who reported having at least one ANC visit and taking at least one IFA tablet was most pronounced among the poorest, those living in rural areas and those living in North province. Overall, this comparison of 2005 and 2010 RDHS data reveals that Rwanda has made remarkable progress in its efforts to improve maternal anemia. During this five year period: (1) the prevalence of anemia among women 15–49 years was reduced by 39 percent, from 28.2 percent to 17.3 percent; (2) the already high ANC coverage rates rose from 94.6 percent to 98.1 percent; and (3) the percentage of women with at least one ANC visit who took iron tablets or syrup increased dramatically from 28.2 percent to 73.0 percent. This evidence shows that the Government of Rwanda has not only substantially reduced the prevalence of anemia nationwide, but that it has done so in a way that is pro-poor and, more generally, in a way that has promoted equity.
Table 1. ANC and IFA Coverage During Last Pregnancy in the Last Five Years by Region, Residence, and Wealth, Rwanda, 2005 and 2010
| Characteristic | No. Women with a Live Birth--Last 5 Years | Received ANC | Took 1 + IFA Tablet | |||
|---|---|---|---|---|---|---|
| 2005 | 2010 | 2005 | 2010 | 2005 | 2010 | |
| Region | ||||||
| Residence | ||||||
| Wealth | ||||||
| City of Kigali | 427 | 635 | 92.7% | 99.1% | 31.0% | 72.0% |
| South | 1,357 | 1,532 | 95.0% | 97.7% | 36.2% | 75.9% |
| West | 1,395 | 1,545 | 92.9% | 98.2% | 33.6% | 71.9% |
| North | 1,052 | 1,035 | 96.7% | 98.5% | 20.6% | 77.8% |
| East | 1,194 | 1,658 | 94.3% | 98.1% | 18.3% | 68.7% |
| Urban | 774 | 819 | 93.0% | 98.4% | 33.8% | 72.5% |
| Rural | 4,651 | 5,586 | 94.7% | 98.1% | 27.2% | 73.1% |
| Lowest 40% | 2,287 | 2,844 | 93.0% | 97.2% | 23.5% | 71.6% |
| Highest 40% | 2,041 | 2,310 | 95.3% | 99.1% | 33.8% | 73.4% |
| National Average | 5,425 | 6,405 | 94.5% | 98.2% | 28.2% | 73.0% |
*unweighted
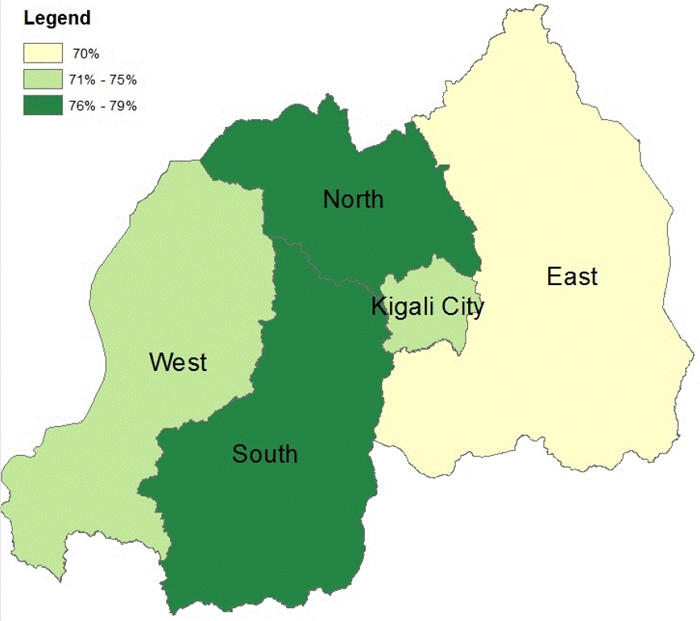
Figure 2. Percentage of Women Who Had at Least One ANC Visit and Received at Least One IFA Tablet by Region, Rwanda, 2010
Analysis by Geographic Regions within Country
The map in Figure 2 shows that there is relatively little regional variation in the proportion of women who had at least one ANC visit and reported receiving any IFA tablets. Rates are slightly lower in the East part of the country than elsewhere—the region with the highest anemia prevalence rates, as mentioned previously. Both these criteria suggest that this part of the country could be prioritized for anemia activities.
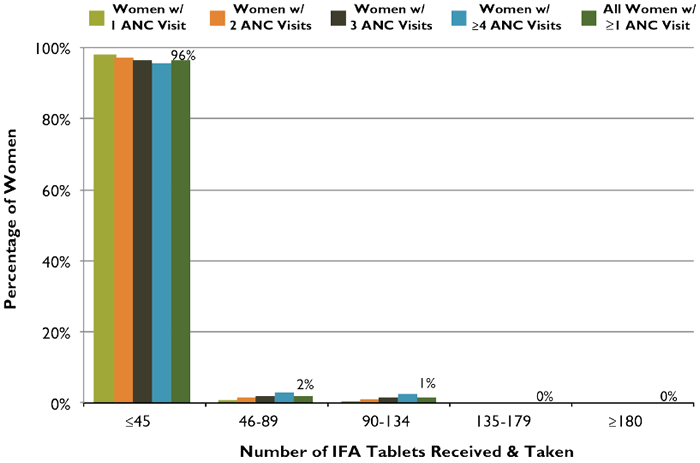
Figure 3. ANC Distribution of IFA Tablets: Number of Tablets Received and Taken According to Number of ANC Visits, Rwanda, 2010
Analysis by Number of ANC Visits
Figure 3 shows the relationship between the number of IFA tablets taken by women who had at least one ANC visit, and the number of ANC visits they had during their last pregnancy. Among women who had at least one ANC visit, 96 percent took at most one-quarter (45) of the ideal minimum number of IFA tablets. Women with more visits were generally likely to receive and take more IFA tablets, but only when the number of tablets received and taken was more than a quarter of the ideal minimum. Even among those women who received IFA tablets and had four or more visits, 95 percent took at most only 45 tablets.
Overall Conclusions and Recommendations
Figure 4 presents the obstacles amongst all women, including those who did not receive ANC during their pregnancy, to taking the ideal minimum number of IFA tablets. In Rwanda, reaching the recommended dosage (following Falter Point 4) seems to be the greatest barrier, though access to and purchase of IFA (Falter Point 2) is also an important barrier.
Taken together, improving the delivery of IFA supplementation in Rwanda relies on identifying and addressing program gaps in IFA supply management and in health workers’ practices. In addition to supply-side factors, modifying women’s long term adherence behaviors and addressing other points mentioned above, under “Analysis of Falter Points” may also lead to more women taking a ideal minimum of 180 tablets.
Despite the great strides that Rwanda has made in the distribution of IFA tablets through its ANC program, this rapid assessment finds that there remains a need to increase the number of pregnant women who take IFA tablets. Formative research may help to identify and prioritize the causes of the as yet unrealized potential of its ANC-based IFA distribution, especially with regards to Falter Points 2 (receiving or purchasing any IFA tablets) and 4 (consumption of at least 180 tablets), so that it can begin to systematically address these shortcomings.
Figure 4. Relative Importance of Each Falter Point in Rwanda: Why Women Who Were Pregnant in the Last Five Years Failed to Take the Ideal Minimum of 180 IFA Tablets
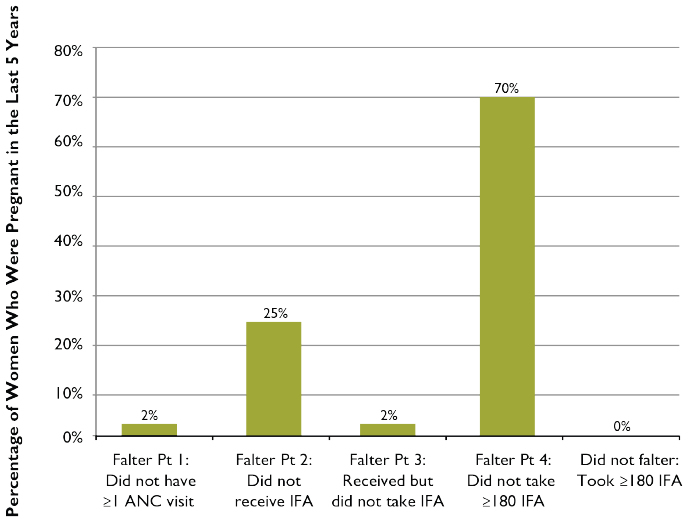
Rwanda has made considerable progress in reducing its maternal mortality ratio (MMR) from 1,071 maternal deaths per 100,000 live births in 2000 to 750 in 2005. An MMR of 476 in 2010, however, remains high (NISR, MOH, and ICF International 2012). While Rwanda is not expected to achieve its Millennium Development Goal 5 (MDG 5A) to reduce the MMR by three-quarters (Abbott and Rwirahira 2010), improving the distribution of IFA through the ANC program could help accelerate progress.
Nearly all ANC visits are conducted in public facilities (NISR, MOH, and ICF International 2012), so Ministry of Health facilities should be the focus of the efforts described above. Improving the distribution of IFA through the ANC program is an important strategy to prevent and control anemia in Rwanda, and to improve the nutrition, health status, and overall mental and physical capacity of women of reproductive age.
Footnotes
1 The WHO categorizes the severity of anemia as a public health problem according to its prevalence: <5%, no public health problem; 5-19.9%, mild; 20-39.9% moderate; ≥40%, severe.
2 The DHS hemoglobin levels used to diagnose the severity of anemia in non-pregnant women are different than those specified by the WHO. The DHS cutoffs for pregnant and non-pregnant women in hemoglobin grams/ deciliter are: Mild 10.0-10.9 (P) 10.0-11.9 (NP); Moderate 7.0-9.9 (P) 7.0- 9.9 (NP); Severe <7.0 (P) <7.0 (NP); Any <11.0 (P) <12.0 (NP).
3 The RDHS asked about IFA tablets or capsules; this brief refers to all types as “tablets”.
4 The RDHS provides a population-based, nationally representative sample of all women in Rwanda.
References
Abbott, Pamela and John Rwirahira. 2010. Millennium Development Goals Rwanda Country Report 2010. Kigali, Rwanda: United Nations Development Programme.
Galloway, Rae. 2003. Anemia Prevention and Control: What Works. Washington, DC: USAID.
Horton, Sue and Jay Ross. 2003. “The Economics of Iron Deficiency.” Food Policy 28(1):51-75.
National Institute of Statistics of Rwanda (NISR) [Rwanda], Ministry of Health (MOH) [Rwanda], and ORC Macro. 2006. Rwanda Demographic and Health Survey 2005. Calverton, Maryland, USA: NISR, MOH, and ORC Macro.
National Institute of Statistics of Rwanda (NISR) [Rwanda], Ministry of Health (MOH) [Rwanda], and ICF International. 2012. Rwanda Demographic and Health Survey 2010. Calverton, Maryland, USA: NISR, MOH, and ICF International.
Stoltzfus, Rebecca J., and Michele L. Dreyfuss. 1998. Guidelines for the use of Iron Supplements to Prevent and Treat Iron Deficiency Anemia. Washington DC: ILSI Press.
Stoltzfus, Rebecca J., Luke Mullany, and Robert E. Black. 2004. “Iron Deficiency Anemia.” In Comparative Quantification of Health Risks: Global and Regional Burden of Disease Attributable to Selected Major Risk Factors, edited by Majid Ezzati, Alan D. Lopez, Anthony Rodgers, and Christopher J. L. Murray, 163-209. Geneva, Switzerland: World Health Organization.
World Health Organization. 2012. Guideline: Daily Iron and Folic Acid Supplementation in Pregnant Women. Geneva, World Health Organization.